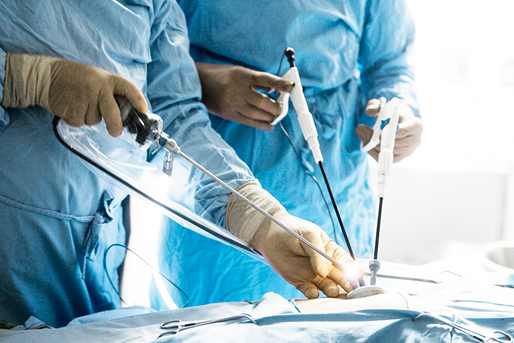
Laparoscopic surgery is a revolutionary surgical technique that utilizes innovative methods to deliver improved surgical outcomes. Through the insertion of short, narrow tubes known as trochars into the abdomen via small incisions, this procedure paves the way for transformative medical possibilities. Surgeons skillfully employ long and narrow instruments within these trochars to manipulate, cut, and suture tissue, granting them great precision. In stark contrast to traditional open abdominal surgery, which necessitates substantial incisions ranging from 6 to 12 inches, laparoscopic surgery embraces a more precise approach. With a mere two to four small incisions measuring half an inch or less, the benefits can be substantial. This technique allows for enhanced visualization and optimal surgical maneuvers. These incisions serve distinct purposes: one acts as an entry point for a camera, while the others accommodate the surgical instruments. A vast array of common surgeries can now be accomplished through laparoscopy, heralding a new era of medical advancement. The procedure entails using a laparoscope, a slender tube equipped with high-intensity light, and a high-resolution camera at its forefront, granting doctors a clear view of the abdominal organs. Guided by these live images projected onto a video monitor, physicians gain invaluable information without resorting to extensive incisions. Moreover, they can extract biopsy samples and perform surgical interventions, all during the same procedure. Eligibility for laparoscopic surgery hinges upon the complexity of an individual’s condition. This technique is rapidly emerging as the preferred choice for an expanding range of common operations, driven by its cost-effective nature and improved patient outcomes. Doctors now recommend laparoscopy to examine various organs, including the liver, appendix, stomach, gallbladder, pancreas, spleen, small and large intestines, and reproductive organs. Exceptional advantages associated with laparoscopic surgery include reduced bleeding, accelerated healing, and diminished pain and scarring. Unlike standard open surgery, recovery time after laparoscopic surgery can be remarkably reduced from several weeks to a few days. A vital aspect contributing to these favorable outcomes is the minimal manipulation of abdominal contents during laparoscopic procedures. Before undergoing most laparoscopic surgeries, patients typically receive general anesthesia. Adequate preparation is vital, and doctors typically advise patients to abstain from eating or drinking for approximately eight hours before the procedure to minimize the risk of anesthesia-induced nausea. In addition, it’s essential to arrange for a reliable means of transportation home considering the potential disorientation resulting from the anesthesia’s effects. Specific instructions regarding medications may also be provided by the attending physician. While laparoscopy generally carries a low-risk profile, it is important to remain vigilant for any potential complications. Although rare, instances of bleeding, infection, or organ damage may occur. If symptoms such as fevers or chills, escalating abdominal pain, redness or discoloration, bleeding, and shortness of breath persist, consult the doctor. Other signs that might warrant a doctor’s attention include swelling, bleeding, continuous nausea or vomiting, inability to urinate, or lightheadedness. There is a minor threat of organ injury during a laparoscopy, which might result in the leakage of blood or other fluids into the body if an organ is accidentally pierced. In such circumstances, additional surgical intervention is required to repair the damage and restore function. Less prevalent risks of laparoscopic surgery include issues from general anesthesia, inflammation of the abdominal wall, and the formation of blood clots that could spread to the pelvis, legs, or lungs. While these dangers are rare, it is critical to be aware of them and get proper medical assistance if any of these symptoms occur.
Karim Sarhane, MD